Introduction: We describe a rare case of chronic compression of the Persistent Median Artery (PMA) in the carpal tunnel resulting in thrombosis and digital ischemia. The case is a 42-year-old male with a cold left index finger and cyanosis. This phenomenon can be referred as, “Persistent Median Artery Compression Syndrome” (PMACS).
Methods: The patient underwent a left upper extremity angiogram. Thrombosis of the PMA was seen and treated with catheter directed thrombolysis, angioplasty and Carpal Tunnel Release (CTR).
Results: The patient was seen by the vascular clinic 18 days after last vascular procedure and plastic surgery clinic 11 days after CTR for postoperative visits at which time he was free of any pain or color changes to the left hand or digits. Aspirin was continued and he was taken off Clopidogrel.
Discussion: Prior to the 8th week of gestation the median artery develops after which the median artery will regress. The median artery may persist and run with the median nerve in the carpal tunnel, this is known as the PMA. A pathologic persistent median artery can be associated with anterior interosseous nerve syndrome, pronator syndrome, CTS and ischemia of the digits. When the digits are threatened by ischemia we advocate a two-tiered treatment approach with initial revascularization followed by surgical release. The pathophysiology, diagnosis and treatment follows the same principles seen in limb ischemia and vascular compression syndromes.
Persistent Median Artery; Digit ischemia; Thrombosed artery; Carpal Tunnel; Compression syndrome
At about 8 weeks gestation, the median artery develops along with the axial artery and interosseous artery, at which time is known to regress, leaving the ulnar and radial arteries as the main blood supply to the hand. In rare instances, the median artery may persist running along with the median nerve in the carpal tunnel, known as a persistent median artery. Although usually asymptomatic, a pathologic persistent median artery has been described in the presence of several risk factors [1-6]. Diagnosis includes a complete history and physical, pulse volume recordings, digital brachial index, ultrasound, computed tomography angiography, and arteriography. Therefore, the pathophysiology, diagnosis and treatment follows the same principles seen in limb ischemia and vascular compression syndromes.
With this case, we describe a 42-year-old male who presented with a cold left index finger and cyanosis. This is a rare case of chronic compression of the Persistent Median Artery (PMA) in the carpal tunnel resulting in thrombosis and digital ischemia. This phenomenon can be referred as, “Persistent Median Artery Compression Syndrome” (PMACS).
A 42-year-old male with hypertension, hyperlipidemia and smokeless tobacco use, was referred by his Primary Care Physician (PCP) to the plastic surgeon for evaluation of a cold left index finger with bluish discoloration for one year that worsened over last 4 days. The patient denied history of trauma, and had no signs of deformities or infection. Compartment syndrome and Carpal Tunnel Syndrome (CTS) were ruled out as he denied any dull aching, paresthesias, weakness or clumsiness. His hand was soft, had no swelling, non-tender, full motor function and no pain with passive movement of the digits. The left index finger was cyanotic in appearance when compared to the other digits, and cool to the touch distal to the Metacarpophalangeal (MCP) joint. Radial and ulnar artery pulses were palpable. The patient had been treated by his PCP with a calcium channel blocker with minimal improvement. Due to the acute change and likely a chronic process a vascular surgeon was consulted. Collectively the concern was ischemia of the digit so he was taken the next day to the operating room for a left upper extremity angiogram (Figure 1). In this first procedure, no interventions were performed as the diagnosis was not initially made. After careful review of the angiography he was found to have thrombosis of a PMA thus ischemia of the digit. Computed tomography angiography was performed and the PMA was identified to be thrombosed in the carpal tunnel. The next day he went to the operating room for a second procedure.
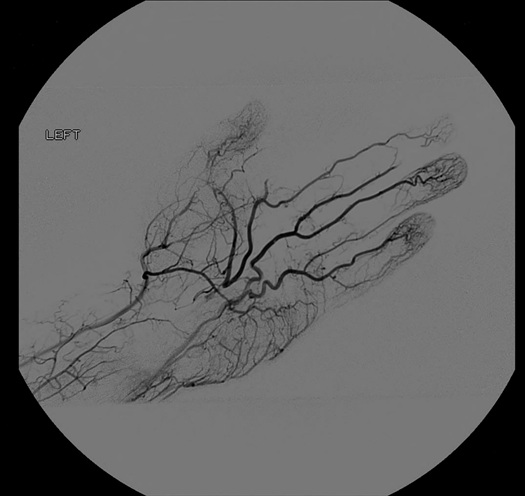
Figure 1. Type I Incomplete Superficial Palmar Arch, Coleman and Anson Classification. Angiogram findings of a patent radial artery in the wrist with one digital vessel to the thumb and forms a diminutive palmar arch to the ulnar side. The ulnar artery is widely patent into the hand and gives digital vessels to the little, ring, and long finger with only collateral contribution to the index finger and thumb. The persistent median artery is seen to be thrombosed in the hand
In the second procedure catheter directed thrombolysis was initiated with tissue plasminogen activator. After 14 hours of lytic therapy the patient returned to the operating room for discontinuation of lytic therapy and percutaneous transluminal angioplasty of the PMA at the level of carpal tunnel. Completion angiogram as shown in Figure 2. Post operatively his hand was pink and warm, motor and sensory were grossly intact and had no signs of ischemia. He was discharged home in stable condition. Five days later he was seen by the plastic surgeon for numbness and tingling of the left hand. After discussions with the vascular surgeon the cause of the patient’s symptoms was surmised to be from chronic compression at the carpal tunnel and would benefit from CTR. The next day the patient underwent a CTR that showed a grossly normal median nerve. Unfortunately, the carpal tunnel was not further explored and the persistent median artery was not searched for during this procedure. The patient was seen by the vascular clinic 18 days after last vascular procedure and plastic surgery clinic 11 days after CTR for postoperative visits at which time he was free of any pain or color changes to the left hand or digits. Aspirin was continued and he was taken off Clopidogrel. He was to return to the plastic surgery clinic in 6 weeks and to the vascular clinic in 6 months but has not returned the either clinic and has been lost to follow up. Institutional Review Board (IRB) approval was obtained prior to undertaking the any investigations involving the patient and case.
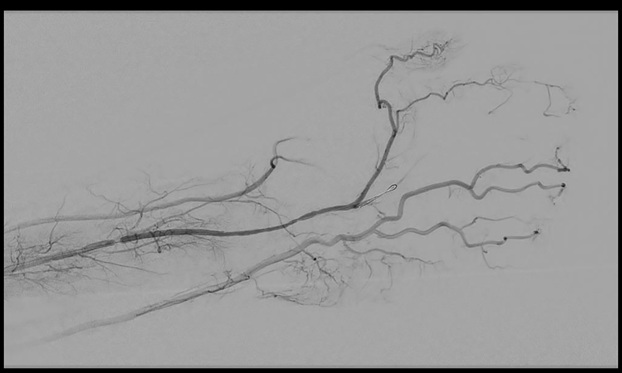
Figure 2. Persistent Median Artery Post Lysis. Angiogram findings of the persistent median artery now open after Fourteen hours of catheter directed thrombolysis therapy and balloon angioplasty
In this case, we describe a 42-year-old male who presented with a cold left index finger and cyanosis. The patient underwent a left upper extremity angiogram. Thrombosis of the PMA was seen and treated with catheter directed thrombolysis, angioplasty and Carpal Tunnel Release (CTR). The patient was seen at follow-up free of pain and digital ischemia. Prior to the 8th week of gestation the median artery develops from the axial artery along with the interosseous artery and supplies the digits in the hands, after which the median artery will regress, leaving the ulnar and radial arteries as the main supply of blood [2]. The median artery may persist and run with the median nerve in the carpal tunnel, this is known as the PMA. The radial, ulnar and PMA when present make up the superficial palmar arch. As suggested by Coleman and Anson, a superficial palmar arch can be complete or incomplete (Figure 3) [3]. In types D and E, the superficial palmar arch includes a PMA and is complete, thus if the PMA is lost due to thrombosis, the digits will continue to be perfused via the radial and ulnar artery collateralization. However, when a PMA is present and the superficial arch is incomplete (type I and J), perfusion to the digits are compartmentalized and rely on a single vessel [3].
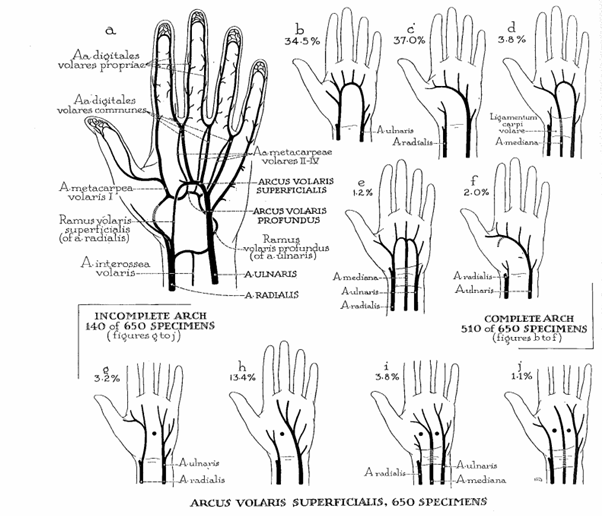
Figure 3. Types of superficial volar arterial arch encountered in 650 dissections [3]
While usually asymptomatic, a pathologic persistent median artery can be associated with anterior interosseous nerve syndrome, pronator syndrome, CTS and ischemia of the digits due to arterial calcification, thrombosis or atherosclerosis. Dickinson and Kleinert described a case of a 46-year-old male with end stage renal failure on hemodialysis that developed extraosseous deposits of calcium in the vessel walls of the PMA resulting in acute CTS [4]. A case of atherosclerosis of the PMA was portrayed by Luyendijk, but no cause stated [5]. Maxwell et al. presented a case of thrombosis of a PMA and median nerve compression in the carpal tunnel from a deep laceration to the thumb resulting in an infection and inflammation in the adventitia of the PMA [6]. In two case studies of digital ischemia, one patient presented with endocarditis, likely resulting in an embolus to the median artery, thrombosis and then ischemia [7]. In the second case, the thrombosis was due to trauma to the hand [8]. In our patient, the risk factors for calcification or atherosclerosis were not present. In addition, on angiography there was no evidence of atherosclerosis or calcifications. There was also no history of trauma, an echocardiogram was negative for thrombus or vegetation, he had no history of atrial fibrillation, myocardial infarction or any other pathology that would be a source of emboli. After excluding these possibilities, using the history and physical and findings from the angiogram we speculated and concluded that the cause was probably due to external compression in the carpal tunnel.
Thus mechanism of compression is similar to other arterial compression syndromes (i.e. median arcuate ligament syndrome, popliteal artery entrapment, thoracic outlet syndrome, hypothenar hammer syndrome…) resulting in end organ ischemia. Depending on the anatomy of the palmar arch this can result in digital ischemia [7,8]. We suggest that thrombosis of the PMA is not likely without underlying pathology. Our patient represents the only description of focal arterial narrowing at the level of the carpal tunnel following catheter directed lytic therapy of a thrombosed PMA. Due to the location we theorize that this narrowing is the result of pathologic changes of the artery due to chronic compression within the carpal tunnel. Continued arterial compression results in a pathway of histologic changes, placed into a 3 stage classification described by Levine et al. for popliteal artery entrapment syndrome. Stage 1 begins with neovascularization and fibrosis involving the adventitia only, in stage 2 the fibrosis progresses into the media and finally in stage 3 the fibrosis extends into the intimal layer resulting in a thrombogenic artery [9].
Diagnosing this persistent median artery compression phenomenon after a history and physical exam suggestive of severe stenosis or occlusion of a palmar artery, not due to emboli, would likely involve the use of pulse volume recordings, digital brachial index, ultrasound, computed tomography angiography, and arteriography. Definitive treatment would follow the same principles as in other vascular compression syndromes. When the digits are threatened by ischemia we advocate a two tiered treatment approach with initial revascularization followed by surgical release of the source of compression (transverse carpal ligament). The use of catheter directed thrombolysis and percutaneous thrombectomy can be utilized as successful first line treatment modalities with the advantage of being performed under sedation without the need for general anesthesia. Other options in conjunction, or alone, include angioplasty, stent, open thrombectomy and/or revascularization with ligation and bypass with vein graft.
Vasculitis, fibromuscular dysplasia, and atherosclerosis all may result in narrowing of an artery ultimately resulting in thrombosis. These diseases have well described angiographic patterns such as calcifications, plaques, ulcerations, vessel irregularities or a beaded appearance, none of which correspond to our patient. We believe the focal arterial stenosis uncovered by catheter directed lysis is angiographically most consistent with a focal fibrosis of the persistent median artery within the carpal tunnel. This is a rare cause of digital ischemia and a diagnosis of exclusion. We are suspicious that some of the previously reported cases of thrombosis of the PMA associated with CTS and digital ischemia may be a result of this compression syndrome. Though exceedingly rare the disease pathophysiology, diagnosis and treatment follows the same principles seen in limb ischemia and other vascular compression syndromes.
- Feigl GC, Petrac M, Pixner T, Ulz H, Mörth C, et al. (2012) The superficial palmar arch and median artery as an example of misleading results due to a small number of investigated specimens or the use of different classifications. Ann Anat. 194: 389-395. [Crossref]
- Tsuruo Y, Ueyama T, Ito T, Nanjo S, Gyoubu H, et al. (2006) Persistent median artery in the hand : A report with a brief review of the literature. Anat Sci Int. 81: 242-252. [Crossref]
- Coleman SS, Anson BJ (1961) Arterial patterns in the hand based upon a study of 650 specimens. Surg Gynecol Obstet. 113: 409-424. [Crossref]
- Dickinson JC, Kleinert JM (1991) Acute carpal-tunnel syndrome caused by a calcified median artery. A case report. J Bone Joint Surg Am. 73: 610-611. [Crossref]
- Luyendijk W (1986) The carpal tunnel syndrome: the role of a persistent median artery. Acta Neurochirurgica. 79: 52-57. [Crossref]
- Maxwell JA, Kepes JJ, Ketchum LD (1973) Acute carpal tunnel syndrome secondary to thrombosis of a persistent median artery. Case report. J Neurosurg. 38: 774-777. [Crossref]
- Beran SJ, Friedman RM, Kassir M (1997) Recurrent digital ischemia due to thrombosis of the persistent median artery. Plast Reconstr Surg. 99: 1169-1171. [Crossref]
- Aulicino PL, Klavans SM, DuPuy TE (1984) Digital ischemia secondary to thrombosis of a persistent median artery. J Hand Surg Am. 9: 820-823. [Crossref]
- Levien LJ, Veller MG (1999) Popliteal artery entrapment syndrome: more common than previously recognized. J Vasc Surg. 30: 587-598. [Crossref]



